The mHealth Summit: Local & Global Converge

“The world is one call away.” – Dr. Feng Zhao, eHealth Coordinator, Africa Health Department, World Bank
*** Welcome! If you’ve come to this page from the HIMSS Definitions of mHealth page or the Wikipedia mHealth page, thank you so much for visiting!
Below I’ve highlighted in orange the definition of mHealth that gets cited a lot. This was from the first ever mHealth Summit, held in back in 2009 in Washington, DC. (This event has gone from 500 people to more than 5,000).
If you’d like a broader definition and understanding of mHealth, take a few minutes to watch this recent video that I’ve added for you. The original post remains after the video. If you have any questions or comments, feel free to leave them below. Thanks again for your time!
* * *
The inaugural mHealth (mobile health) Summit was recently held in Washington, D.C. Hosted by the Foundation for the National Institutes of Health with partnering sponsor Microsoft Research, the Summit mission was “to explore the use of mobile technologies to improve public health, particularly regarding underserved populations; health research, training, and education applications; and delivery systems, in the U.S. and around the world.” The World Bank Day @ mHealth Summit served as a warm-up act the preceding day.
As defined at the meeting, mHealth is “the delivery of healthcare services via mobile communication devices.” Much more than just a subset of eHealth, mHealth offers an unparalleled opportunity to reach individuals and affect change. After three days of incredible talks by passionate experts, I was struck by several themes and future directions.
The individual is at the center
The applications that really work and really make a difference all start with the needs of individuals, whether they are patients or healthcare workers. A need is recognized, and at some point mobile technology is viewed as potentially playing a role in a solution. This seems incredibly intuitive, but it can be tempting to do the opposite: start with a killer technology and then go in search of an issue to solve with it.
In parallel to this, the technologies that ultimately work well are the ones that undergo extensive iterations based on user needs (for example, redesigning misunderstood icons). It was repeatedly (and I mean repeatedly!) stressed that mHealth is not about technology, but about how to use it.
“At the end of the day, it’s health that’s important, not eHealth.” – Dr. Souheil Marine, Head of ICT Application and Cybersecurity, International Telecommunication Union
Knowledge is power
Mobile technology offers access, access provides knowledge, and knowledge bestows power. There is an expanding list of exemplary mHealth programs that have empowered individuals to take a more active role in their health and well being, and of the health of those around them. Thus there is a substantial need for credible, trustworthy, understandable, concise health information that is relevant, culturally sensitive, and actionable.
Personalized medicine redefined
Personalized medicine has been defined as “an emerging practice of medicine that uses an individual’s genetic profile to guide decisions made in regard to the prevention, diagnosis, and treatment of disease. Knowledge of a patient’s genetic profile can help doctors select the proper medication or therapy and administer it using the proper dose or regimen.” The mantra for this type of personalized medicine is typically: right drug, right dose, right purpose, right time, right person. It’s personalization based on cellular DNA.
mHealth expands the definition of personalized medicine while maintaining the context of the individual: right person, right information, right place, right time. Mobile means anytime and anywhere, at the discretion of the individual. It’s personalization based on cell phone DNA.
Communicable and noncommunicable diseases
Presentations highlighted mHealth programs to address infectious diseases such as HIV/AIDS and tuberculosis, as well chronic noncommunicable diseases (NCDs) which include heart disease, stroke, chronic lung diseases, diabetes, and cancers. NCDs kill more than twice as many individuals worldwide as the number of those that die from infectious diseases, maternal and perinatal conditions, and nutritional deficiencies combined. NCDs account for about 60% of all deaths globally and 80% of these deaths occur in low- and middle-income countries. A World Health Organization global report notes it is the “invisible” epidemics of NCDs that will take the greatest toll in deaths and disability for the foreseeable future.
As mHealth programs and tools are further developed to combat both communicable and noncommunicable diseases, it will become increasingly important to share best practices, messaging, outcomes, and lessons learned with respect to education, prevention, screening, treatment, and management. These conditions do not exist in isolation in individuals and should not be addressed in isolation.
Literacy: Can you read me now?
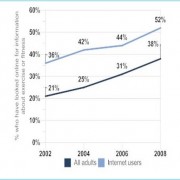
General literacy and health literacy remain huge issues. Almost a quarter of adults possess no more than the most simple and concrete literacy skills in the United States. Over one third of adult Americans have basic or below basic health literacy, which is defined as “the degree to which individuals have the capacity to obtain, process, and understand basic health information and services needed to make appropriate health decisions.” Poor health literacy is associated with a failure to seek preventive care, medication and treatment errors, higher rates of hospitalization, and higher use of emergency services.
The use of iconography and outreach to family members and friends were mentioned as ways to overcome literacy and language barriers (children often translate for their parents). mHealth offers an exciting platform by which to develop new tools and messaging strategies that don’t require a high level of literacy and also to develop programs to increase health literacy in a targeted, non-stigmatizing, non-threatening manner.
Senses and dimensions
The mobile communication strategies highlighted during the meetings most often featured icons and text, with some photos and a bit of video. The human senses that these engage are vision and hearing (excluding the touch of pushing buttons). In this sense, mHealth is in its infancy – it relies on 2 senses and 2 dimensions to communicate (3 dimensions if you include time). Imagine the future of telemedicine: 3-dimensional imaging, and biomarkers and sensors that detect and transmit smell, taste and touch. Multi-sensory, multi-dimensional technology will exponentially increase accuracy and engagement; further increase compliance and outcomes; and bridge languages, literacy, and cultures.
“What used to take up a building now fits in my pocket, and what fits in my pocket will fit inside a blood cell in 25 years.” – Ray Kurzweil, inventor and futurist
The inaugural mHealth Summit was a huge success and portends an exciting future. What do you envision for the future of mHealth?
mHealth Summit Commentaries
- Learnings from mHealth Summit John Moore, Chilmark Research
- World Bank Day @ mHealth Summit – Aftermath Florian Sturm, ICT4D.at
- mHealth Summit: HHS sees enormous potential Brian Dolan, Mobihealthnews
mHealth Reports & Related Features
- mHealth for Development: The opportunity of mobile technology for healthcare in the developing world. (PDF) UN Foundation-Vodafone Foundation Partnership, 2009.
- 2008-2013 Action plan for the global strategy for the prevention and control of noncommunicable diseases. (PDF) World Health Organization, Geneva, 2008.
- Public policy and the challenge of chronic noncommunicable diseases. (PDF) Adeyi O, Smith O, Robles S. The World Bank, Washington, D.C., 2007.
- The pocket spy: Will your smartphone rat you out? Gedes, L. New Scientist, 14 Oct 2009.
- Mobile marvels. A special report on telecoms in emerging markets. The Economist, Sept 24, 2009.
mHealth Resources
- AppLab: Transforming Lives through Innovation in Information Access
- eMOCHA: electronic Mobile Open-source Comprehensive Health Application
- EpiSurveyor: Data collection on mobile phones made incredibly simple
- GeoChat: Integrating mobile field communications with situational awareness
- WISER: the Wireless Information System for Emergency Responders
Mark your calendars: Next year’s Summit will be Nov 9-10, in Washington, D.C.
Twitter hashtags: World Bank Day #mHealth09; mHealth Summit #mHS09
A special thank you to those who took the time to tweet the meetings, write up reviews, and share insights, photos and videos. The mHealth crowd is incredibly sharp, passionate, and engaged, and I look forward to future discussions.
Posts from other mHealth Summits
- mHealth Summit 2010: A context check list
- The 2011 mHealth Summit Summed Up in 5 Quotes, Words and Companies, Plus 1 Jacket
- 8 Themes from the 2012 mHealth Summit







Thanks for your take on the mHealth Summit–great highlights–“it is about health”–amazing group of innovators and ideas on how to improve health worldwide. Appreciate, as always your grasp of the critical pieces.
Lindsey